Welcome to the California Health Facility Information Database (Cal Health Find), a multi-purpose source of information on the more than 10,000 health-care facilities regulated by the California Department of Public Health (CDPH). Cal Health Find provides health care consumers and providers with information about licensed and certified facilities throughout California. The web site's content is made available by CDPH's Center for Health Care Quality and its
Licensing and Certification Division (L&C).
Cal Health Find is a user-friendly tool that makes it easy to:
- Search for facilities by name, facility type or location.
- View provider details, including facility ownership, licensing and certification status (acceptance of Medicare and/or Medi-Cal), and performance history (complaints, entity/facility reported incidents, state enforcement actions, and deficiencies identified by L&C staff).
- Compare up to three facilities at a time.
- File a complaint electronically.
Table of Contents
Administrative Penalty
A civil monetary penalty in an amount up to $125,000 per violation or deficiency constituting an immediate jeopardy to the health and safety of a patient. (Ref: Health and Safety Code section 1280.1 and 1280.3).
Administrator
In a nursing home or facilities for the developmentally disabled, the administrator is a person licensed as a nursing home administrator; in other health care settings, the administrator is a person appointed the responsibility for overseeing the services, functions and operations.
Adverse Event
Includes any of the following:
(1) Surgical events, including the following: (A) Surgery performed on a wrong body part that is inconsistent with the documented informed consent for that patient. A reportable event under this subparagraph does not include a situation requiring prompt action that occurs in the course of surgery or a situation that is so urgent as to preclude obtaining informed consent. (B) Surgery performed on the wrong patient. (C) The wrong surgical procedure performed on a patient, which is a surgical procedure performed on a patient that is inconsistent with the documented informed consent for that patient. A reportable event under this subparagraph does not include a situation requiring prompt action that occurs in the course of surgery, or a situation that is so urgent as to preclude the obtaining of informed consent. (D) Retention of a foreign object in a patient after surgery or other procedure, excluding objects intentionally implanted as part of a planned intervention and objects present prior to surgery that are intentionally retained. (E) Death during or up to 24 hours after induction of anesthesia after surgery of a normal, healthy patient who has no organic, physiologic, biochemical, or psychiatric disturbance and for whom the pathologic processes for which the operation is to be performed are localized and do not entail a systemic disturbance.
(2) Product or device events, including the following: (A) Patient death or serious disability associated with the use of a contaminated drug, device, or biologic provided by the health facility when the contamination is the result of generally detectable contaminants in the drug, device, or biologic, regardless of the source of the contamination or the product. (B) Patient death or serious disability associated with the use or function of a device in patient care in which the device is used or functions other than as intended. For purposes of this subparagraph, "device" includes, but is not limited to, a catheter, drain, or other specialized tube, infusion pump, or ventilator. (C) Patient death or serious disability associated with intravascular air embolism that occurs while being cared for in a facility, excluding deaths associated with neurosurgical procedures known to present a high risk of intravascular air embolism.
(3) Patient protection events, including the following: (A) An infant discharged to the wrong person. (B) Patient death or serious disability associated with patient disappearance for more than four hours, excluding events involving adults who have competency or decision making capacity. (C) A patient suicide or attempted suicide resulting in serious disability while being cared for in a health facility due to patient actions after admission to the health facility, excluding deaths resulting from self-inflicted injuries that were the reason for admission to the health facility.
(4) Care management events, including the following: (A) A patient death or serious disability associated with a medication error, including, but not limited to, an error involving the wrong drug, the wrong dose, the wrong patient, the wrong time, the wrong rate, the wrong preparation, or the wrong route of administration, excluding reasonable differences in clinical judgment on drug selection and dose. (B) A patient death or serious disability associated with a hemolytic reaction due to the administration of ABO-incompatible blood or blood products. (C) Maternal death or serious disability associated with labor or delivery in a low-risk pregnancy while being cared for in a facility, including events that occur within 42 days post-delivery and excluding deaths from pulmonary or amniotic fluid embolism, acute fatty liver of pregnancy, or cardiomyopathy. (D) Patient death or serious disability directly related to hypoglycemia, the onset of which occurs while the patient is being cared for in a health facility. (E) Death or serious disability, including kernicterus, associated with failure to identify and treat hyperbilirubinemia in neonates during the first 28 days of life. For purposes of this subparagraph, "hyperbilirubinemia" means bilirubin levels greater than 30 milligrams per deciliter. (F) A Stage 3 or 4 ulcer, acquired after admission to a health facility, excluding progression from Stage 2 to Stage 3 if Stage 2 was recognized upon admission. (G) A patient death or serious disability due to spinal manipulative therapy performed at the health facility.
(5) Environmental events, including the following: (A) A patient death or serious disability associated with an electric shock while being cared for in a health facility, excluding events involving planned treatments, such as electric counter shock. (B) Any incident in which a line designated for oxygen or other gas to be delivered to a patient contains the wrong gas or is contaminated by a toxic substance. (C) A patient death or serious disability associated with a burn incurred from any source while being cared for in a health facility. (D) A patient death associated with a fall while being cared for in a health facility. (E) A patient death or serious disability associated with the use of restraints or bedrails while being cared for in a health facility.
(6) Criminal events, including the following: (A) Any instance of care ordered by or provided by someone impersonating a physician, nurse, pharmacist, or other licensed health care provider. (B) The abduction of a patient of any age. (C) The sexual assault on a patient within or on the grounds of a health facility. (D) The death or significant injury of a patient or staff member resulting from a physical assault that occurs within or on the grounds of a facility.
(7) An adverse event or series of adverse events that cause the death or serious disability of a patient, personnel, or visitor.
(c) The facility shall inform the patient or the party responsible for the patient of the adverse event by the time the report made.
(d) "Serious disability" means a physical or mental impairment that substantially limits one or more of the major life activities of an individual, or the loss of bodily function, if the impairment or the loss lasts more than seven days or is still present at the time of discharge from an inpatient health care facility, or the loss of a body part. (Ref: Health and Safety Code section 1279.1)
Appeals
Legal hearing in which a licensee may attempt to refute an enforcement action issued by the Department against a facility.
Automated Survey Processing Environment (ASPEN)
ASPEN Central Office (ACO) is a Windows®-based program that enables state agencies to implement information-based administration of the health care facilities under their supervision. ACO stores data about certified facilities regulated by the Centers for Medicare and Medicaid Services (CMS) and the regulations pertinent to those facilities.
No Listings
Citations
Civil sanctions against long-term health care facilities in violation of state and federal laws and regulations relating to patient care. (Ref: Health and Safety Code section 1423).
Read more in About Citations.
Client
A person who is receiving services from an intermediate care facility for the developmentally disabled.
Complainant
Any person that files a complaint about an alleged violation of applicable requirements or noncompliance with federal and/or state laws and regulations.
Complaint
A report made to the state agency or regional office by anyone other than the administrator or authorized official for a provider or supplier that alleges noncompliance of federal and/or state laws and regulations. (Ref: Health and Safety Code section 1420).
Consultant
Staff in the Licensing and Certification Program Professional Consultants who provide medical, medical record, nutrition, pharmacy, and occupational therapy consultation services.
Deficiencies
Violations of federal and/or state laws and regulations that CDPH cites during the course of a survey.
Entity Reported Incident
Federal term for an official notification to L&C from a self-reporting facility or health care provider (i.e., the administrator or authorized official for the provider) that alleges noncompliance of federal and/or state laws and regulations. Also known as Facility Reported Incident.
Evaluator
Staff in the Licensing and Certification Program that are trained to conduct complaint investigations, inspections and surveys, formally classified as Health Facility Evaluator Nurses.
No Listings
No Listings
No Listings
Immediate Jeopardy
An allegation or violation where the noncompliance with federal or state laws and regulations has caused or is likely to cause serious injury, harm, impairment, or death to residents, patients, or clients.
Immediate and Serious Threat
A situation or complaint where the noncompliance with state laws and regulations has a threat of imminent danger of death or serious bodily harm.
No Listings
No Listings
Licensee
The person, persons, firm, partnership, association, corporation, political subdivision of the State, or other governmental agency to whom a license has been issued to operate a health facility or agency.
Long-Term Health Care Facility
(a)"Long-Term health care facility" means any facility licensed pursuant to Health and Safety Code Chapter 2 (commencing with section 1250) that is any of the following:
- Skilled nursing facility.
- Intermediate care facility.
- Intermediate care facility/developmentally disabled.
- Intermediate care facility /developmentally disabled habilitative.
- Intermediate care facility/developmentally disabled nursing.
- Congregate living health facility.
- Nursing facility.
- Intermediate care facility/developmentally disabled-continuous nursing.
(b) “Long-term health care facility” also includes a pediatric day health and respite care facility. (Ref: Health and Safety Code section 1760).
(c) “Long-term health care facility” does not include a general acute care hospital or an acute psychiatric hospital, except for that distinct part of the hospital that provides skilled nursing facility, intermediate care facility, intermediate care facility/developmentally disabled, or pediatric day health and respite care facility services (Ref: Health and Safety Code section 1418(c)).
Medical Breach
The unlawful or unauthorized access to, and use or disclosure of, a patient’s medical information. (Ref: Health and Safety Code section 1280.15(a)).
Non-Long Term Care Facility
A health care facility or agency that is not a long-term care facility (for example, a general acute care hospital, clinic, or acute psychiatric hospital), required to be licensed pursuant to state law.
No Listings
Patient
A person under medical treatment in a health care facility, provider or agency.
No Listings
Resident
A person who is receiving skilled nursing services and resides in a nursing home. (Patient, resident, client are often used interchangeably)
Substandard Quality of Care
Noncompliance with federal laws and regulations for nursing home residents that present as immediate jeopardy or harm to resident health or safety.
Substantiated
Any allegation that is part of a complaint, that did occur, and was verified by evidence. An allegation is considered substantiated based on the finding about the individual or specified situation named by the complainant.
Substantiated Allegation with No Regulatory Violation
Substantiated allegations that do not constitute a violation of laws or regulations enforced by L&C. These allegations may be forwarded to another agency for investigation if appropriate.
Survey Closure Date
The date that all activities associated with the complaint investigation are finished. This includes activities conducted at the health facility’s site as well as activities conducted in the district office.
No Listings
Unsubstantiated
Any allegation where evidence cannot support that the allegation did occur. Unsubstantiated allegations can be due to the allegation not occurring or lack of sufficient evidence to support the allegation.
No Listings
No Listings
No Listings
No Listings
No Listings
About Cal Health Find:
The California Health Facility Information Database or Cal Health Find is a website that provides immediate access to information about California’s licensed health care facilities. The website includes facility profile information, such as ownership, licensing status, certification status (acceptance of Medicare and/or Medi-Cal), and performance history including complaints, entity/facility reported incidents, state enforcement actions, and deficiencies identified by the California Department of Public Health (CDPH) Licensing and Certification Program (L&C) staff.
Additionally, the Statements of Deficiencies/Plans of Correction (Form 2567) approved after March 23, 2011, are displayed on the webpage for the individual skilled nursing facility.
Facilities can be located by entering a ZIP code, city, or county; a map of the surrounding area will be displayed. Complaints regarding specific facilities may be submitted through Cal Health Find.
The information displayed in Cal Health Find comes from data recorded in the federal Automated Survey Processing Environment (ASPEN) system and the state Electronic Licensing Management System (ELMS).
Cal Health Find displays complaints and entity/facility reported incidents by year and under the Intake Received Date (e.g. Year 2009, Year 2010). The Intake Received Date is the date CDPH received the complaint or entity/facility reported incident and may be different from the date an incident occurred or different from the date the facility reported the incident to CDPH. For example, reports e-mailed to CDPH after hours on Friday would have an Intake Received Date of the next working day.
Cal Health Find displays complaint and entity/facility reported incidents only after the investigation has concluded. In some cases, the investigation closure may be significantly delayed due to law enforcement involvement or unavailable records (such as coroner reports). Once the investigation is concluded, it will be displayed in Cal Health Find under the year of the date it was originally received by CDPH.
For complaints and entity/facility reported incidents that result in a state citation (i.e. AA, A or B citation), Cal Health Find displays the enforcement action under the date the citation was issued to the facility. Therefore, an incident may be displayed in two places: (1) Under the year of the Intake Received Date, and (2) under the year the citation was issued.
A class AA citation is a violation that CDPH "determines to have been a substantial factor in the death of a resident of a long term care facility.” In any action to enforce a class AA citation, CDPH must prove the violation was a substantial factor in the death and the death resulted from an occurrence of a nature that the regulation was designed to prevent (Health and Safety Code Section 1424(c)).
All long-term care facilities may receive class AA citations.
CDPH conducts a thorough investigation of the event using principals of documentation that include record reviews, direct observations and interviews. The CDPH District Office manager reviews the investigation report. If the manager concurs the violation rises to the level of a class AA violation, the findings are submitted to a CDPH medical consultant, the Office of Legal Services, and the Field Operations Branch Chief for review and approval. If all reviewers concur with the findings, the District Office issues the citation to the facility.
Yes, the citation can either be appealed directly to court or to an administrative hearing unit. The outcome of the citation and collection of any fines assessed are not final until all appeals have been exhausted (Health and Safety Code Section 1428(b).
Health and Safety Code Section 1424.5 (a)(1) dictates the minimum fine that can be assessed for a class AA citation is $30,000 and the maximum fine is $120,000. Facilities that do not contest the level of the citation or the amount of the fine may, within 30 days of the citation issuance, pay 65 percent of the assessed fine (Health and Safety Code Sections 1424.5(b).
All money collected from citations is deposited in the Health Facilities Citation Penalties Account and used for quality assurance initiatives that directly improve the health care and services offered to long term care facility residents (Health and Safety Code Section 1417.2).
Yes. For a second or subsequent class AA citation within a 24-month period that has been sustained following a citation review conference, or where the licensee has chosen not to exercise its right to a citation review conference, CDPH shall commence action to suspend or revoke the facility’s license. (Health and Safety Code Section 1424.5(a)(1)).
The table below displays the classes of the various state citations as well as the criteria needed to classify the level of the citation.
| AA |
LTC |
- Violations that meet the criteria for a class "A" violation, and
- That the department determines to have been a substantial factor in the death of a resident of a long-term health care facility.
|
| A |
LTC |
- Imminent danger of death or serious harm to patients, or
- A substantial probability of death or serious physical harm to patients.
|
| B |
LTC |
- Has a direct or immediate relationship to patient health, safety, or security.
- Can include emotional and financial elements.
|
| Patient Rights B |
LTC |
- Any violation of patient’s rights as described in Title 22 of the California Code of Regulations.
- A patient’s rights violation produces a situation likely to cause significant humiliation, indignity, anxiety, or other emotional trauma, but is not serious enough to be a Class "A," unless CDPH determines such a violation meets the criteria of a Class "A".
|
| Abuse Reporting B |
LTC |
- Failure of the facility to report incidents of alleged or suspected abuse of a facility resident.
- Must be reported to CDPH immediately or within 24 hours of the incident.
- Failure of the facility to meet the requirements in Health and Safety Code 1418.91 results in a Class “B” citation.
|
| Financial Occurrence Reporting B |
SNF |
- Failure of the licensee to notify CDPH of financial occurrences as described in Health and Safety Code 1421.1.
- CDPH must be notified within 24 hours of occurrence.
- Notification to CDPH may be in written form if it is provided by FAX or overnight mail, or by telephone with a written confirmation within five calendar days.
|
| Posting Notice of Imposed Remedies B |
LTC |
- Facility failure to post notice of remedies imposed for violation(s) of state or federal requirements as described in Health and Safety Code 417.15 will result in a Class "B" citation.
|
| Written Notice of Imposed Remedies B |
SNF |
- Written notification of imposed remedies must be given to the following: each resident, each resident’s responsible party and legal representative, and all applicants for admission to the facility.
- Facility failure to provide written notice of imposed remedies as described in Health and Safety Code 1429.1 will result in a Class "B" citation.
|
| Posting of Ombudsman Information A & B |
SNF |
CDPH shall assess a civil penalty of $100 for each day the facility fails to post the Ombudsman information poster (pursuant to Section 9718 of the Welfare and Institutions Code).
- Issued and enforced in the same manner as a Class "B" citation when the penalty is assessed at less than $2,000.
- Issued and enforced in the same manner as a Class "A" citation when the assessed penalty is equal to or in excess of $2,000.
|
| Willful Material Falsification (WMF) |
LTC |
Any entry in the health care record that falsely reflects the condition/care/services provided to the resident, such as:
- Administration of medication or treatments ordered.
- Services pertaining to the prevention or treatment of pressure sores or contractures.
- Tests and measurements of vital signs.
- Notations of fluid input and output.
|
| Retaliation/ Discrimination |
LTC |
Prohibits licensee from discriminating or retaliating against:
- Patient
- Employee
- Any other person who has presented a grievance/complaint, or has initiated/cooperated in any investigation/preceding of any governmental entity relating to care/services/conditions.
|
| C (written as state deficiencies) |
LTC |
The violation at the time of the occurrence has minimal (remote) relationship to patient health, safety or security. |
| Willful Material Omission (WMO) |
LTC |
- Willful failure to record any untoward event which has affected the health, safety, or security of a patient, and
- Was omitted with the knowledge that the record falsely reflects the condition of the patient or care or services provided.
|
| Family Council B |
SNF |
- Facility may not prohibit the formation of a family council.
- Facility may not limit the function of the family council.
- Failure of the facility to meet the requirements of Health and Safety Code 1418.4 results in a Class "B" citation.
|
An administrative penalty (AP) is a monetary penalty issued for a facility’s violation of the requirements of licensure that impacts, or is likely to impact, the health and safety of patients. A penalty can be issued in an amount of up to $75,000 for a first deficiency constituting an immediate jeopardy (IJ) to the health and safety of a patient, up to $100,000 for the second subsequent IJ deficiency, and up to $125,000 for a third and every subsequent IJ deficiency (Health and Safety Code (HSC) section 1280.3). APs for non-IJ licensing deficiencies can be assessed in an amount up to $25,000. CDPH's L&C program completes investigations of these deficiencies and assesses penalties for those violations as applicable.
An immediate jeopardy is a situation in which the hospital’s noncompliance with one or more requirements of licensure has caused, or is likely to cause, serious injury or death to the patient.
Only general acute care hospitals; acute psychiatric hospitals; and special hospitals are affected by these laws.
The administrative penalties are the first to be issued by CDPH under new authority granted by Health and Safety Code section 1280.1 (Senate Bill 1312, Statutes of 2006, Chapter 895), which was signed by Governor Arnold Schwarzenegger last year and became effective on January 1, 2007.
The fines are to be deposited in the Licensing and Certification Program Fund established pursuant to H&S 1266.9. This is a special fund for L&C.
The recommendation to issue an administrative penalty is made at the L&C District Office level by the investigating surveyor and their supervisor after review of the investigation and approval of the determination to issue the administrative penalty. These proposed/recommended penalties are sent to Office of Legal Services and the L&C Deputy Director for approval and issuance. The Deputy Director of L&C makes the final decision.
No, not at this time. The determination to terminate a license is made after investigations and assessments of a facility’s ability and capacity to implement plans of correction to assure the health and safety of patients is protected. The determinations also take into account the severity of the deficiencies/violations that occurred, the ability to implement corrections and their assurance, through demonstration and assessment, that such occurrences will not happen in the future.
Facilities can appeal the administrative penalties by requesting a hearing within 10 calendar days of notification. If a hearing is requested, the penalties are to be paid if upheld following appeal. In addition to the penalties, the facility is required to implement a plan of correction to prevent future incidents.
No. The law also allows for fines of up to $25,000 for violations that do not rise to the level of immediate jeopardy.
About Adverse Events:
An adverse event is defined as a medical occurrence that caused or is an ongoing threat of imminent danger of death or serious bodily harm at an acute general hospital, acute psychiatric hospital and special hospital. There are 28 “Adverse Events” defined by SB 1301 and appear under the following headings:
- Surgical events
- Product or device events
- Patient protection events
- Care management events
- Environmental events
- Criminal events
- An adverse event or series of adverse events that cause the death or serious disability of a patient, personnel, or visitor.
Legislation (SB 1301) was enacted in July 2007 due to a heightened awareness of the problem of preventable medical errors in hospitals. The new law’s intent is to promote safety by increasing government oversight and providing public disclosure of medical errors both to the affected patient and public.
The reporting of adverse events applies to the following types of facilities:
- General Acute Care Hospitals (GACH)
- Acute Psychiatric Hospitals (APH)
- Special Hospitals (SH)
There are 28 adverse events defined by the Health and Safety Code, Section 1279.1 (b) (1) – (7) and reflects the following:
- Surgical events, including the following:
- A. Surgery performed on a wrong body part that is inconsistent with the documented informed consent for that patient. A reportable event under this subparagraph does not include a situation requiring prompt action that occurs in the course of surgery or a situation that is so urgent as to preclude obtaining informed consent.
- B. Surgery performed on the wrong patient.
- C. The wrong surgical procedure performed on a patient, which is a surgical procedure performed on a patient that is inconsistent with the documented informed consent for that patient. A reportable event under this subparagraph does not include a situation requiring prompt action that occurs in the course of surgery, or a situation that is so urgent as to preclude the obtaining of informed consent.
- D. Retention of a foreign object in a patient after surgery or other procedure, excluding objects intentionally implanted as part of a planned intervention and objects present prior to surgery that are intentionally retained.
- E. Death during or up to 24 hours after induction of anesthesia after surgery of a normal, healthy patient who has no organic, physiologic, biochemical, or psychiatric disturbance and for whom the pathologic processes for which the operation is to be performed are localized and do not entail a systemic disturbance.
- Product or device events, including the following:
- A. Patient death or serious disability associated with the use of a contaminated drug, device, or biologic provided by the health facility when the contamination is the result of generally detectable contaminants in the drug, device, or biologic, regardless of the source of the contamination or the product.
- B. Patient death or serious disability associated with the use or function of a device in patient care in which the device is used or functions other than as intended. For purposes of this subparagraph, "device" includes, but is not limited to, a catheter, drain, or other specialized tube, infusion pump, or ventilator.
- C. Patient death or serious disability associated with intravascular air embolism that occurs while being cared for in a facility, excluding deaths associated with neurosurgical procedures known to present a high risk of intravascular air embolism.
- Patient protection events, including the following:
- A. An infant discharged to the wrong person.
- B. Patient death or serious disability associated with patient disappearance for more than four hours, excluding events involving adults who have competency or decision making capacity.
- C. A patient suicide or attempted suicide resulting in serious disability while being cared for in a health facility due to patient actions after admission to the health facility, excluding deaths resulting from self-inflicted injuries that were the reason for admission to the health facility.
- Care management events, including the following:
- A. A patient death or serious disability associated with a medication error, including, but not limited to, an error involving the wrong drug, the wrong dose, the wrong patient, the wrong time, the wrong rate, the wrong preparation, or the wrong route of administration, excluding reasonable differences in clinical judgment on drug selection and dose.
- B. A patient death or serious disability associated with a hemolytic reaction due to the administration of ABO-incompatible blood or blood products.
- C. Maternal death or serious disability associated with labor or delivery in a low-risk pregnancy while being cared for in a facility, including events that occur within 42 days post delivery and excluding deaths from pulmonary or amniotic fluid embolism, acute fatty liver of pregnancy, or cardiomyopathy.
- D. Patient death or serious disability directly related to hypoglycemia, the onset of which occurs while the patient is being cared for in a health facility.
- E. Death or serious disability, including kernicterus, associated with failure to identify and treat hyperbilirubinemia in neonates during the first 28 days of life. For purposes of this subparagraph, "hyperbilirubinemia" means bilirubin levels greater than 30 milligrams per deciliter.
- F. A Stage 3 or 4 ulcer, acquired after admission to a health facility, excluding progression from Stage 2 to Stage 3 if Stage 2 was recognized upon admission.
- G. A patient death or serious disability due to spinal manipulative therapy performed at the health facility.
- Environmental events, including the following:
- A. A patient death or serious disability associated with an electric shock while being cared for in a health facility, excluding events involving planned treatments, such as electric countershock.
- B. Any incident in which a line designated for oxygen or other gas to be delivered to a patient contains the wrong gas or is contaminated by a toxic substance.
- C. A patient death or serious disability associated with a burn incurred from any source while being cared for in a health facility.
- D. A patient death associated with a fall while being cared for in a health facility.
- E. A patient death or serious disability associated with the use of restraints or bedrails while being cared for in a health facility.
- Criminal events, including the following:
- A. Any instance of care ordered by or provided by someone impersonating a physician, nurse, pharmacist, or other licensed health care provider.
- B. The abduction of a patient of any age.
- C. The sexual assault on a patient within or on the grounds of a health facility.
- D. The death or significant injury of a patient or staff member resulting from a physical assault that occurs within or on the grounds of a facility.
- An adverse event or series of adverse events that cause the death or serious disability of a patient, personnel, or visitor.
Requires general acute care hospitals, acute psychiatric hospitals and special hospitals to report an adverse event to the Department of Public Health no later than five (5) days after the adverse event has been detected, or, if that event is an ongoing urgent or emergent threat to the welfare, health, or safety of patients, personnel, or visitors, not later than 24 hours after the adverse event has been detected. Licensing and Certification Program is required to conduct an on-site investigation of all reported adverse events.
The California Department of Public Health may assess a civil penalty in an amount not to exceed $100 for each day that the adverse event is not reported following the initial five-day period or 24-hour period.
About Complaints and Surveys:
An entity/facility reported incident is any report made to CDPH by a representative of a health care facility authorized to speak on behalf of the facility. Facilities are required to report unusual occurrences. Unusual occurrences may include epidemics, outbreaks, disasters, fires, disruption of services, major accidents or unusual occurrences that threaten the health and safety of patients, residents, clients, staff or visitors.
A complaint is a report received by CDPH for anything other than an entity/facility reported incident. All complaints are anonymous; the identity of the person that made the complaint is not shared with the facility.
Entity/Facility reported incidents and complaints are investigated in the same manner.
Unsubstantiated finding – Any complaint or entity/facility reported incident where evidence does not support the event occurred. A finding that is unsubstantiated can be due to the fact that an incident did not occur or a lack of sufficient evidence to support that it did occur.
Substantiated finding – Any complaint or entity/facility reported incident that has sufficient evidence to support the event occurred. However, substantiated does not mean a federal and/or state deficiency occurred because there may not have been a violation of federal and/or state regulations or statutes.
When an investigation, through observation, interviews, and clinical record review, determines a deficient practice (State or Federal violation) occurred.
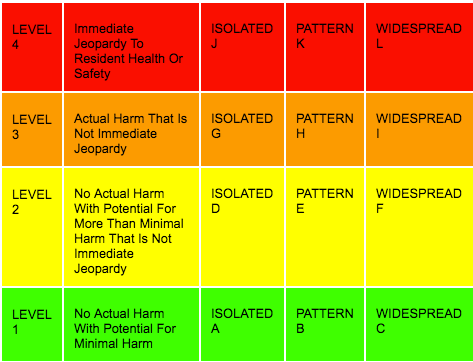
The "scope and severity" of a federal deficiency is based on how egregious the violation was ("A" being minimal and "L" the most severe) and how widespread the problem was in terms of the affected residents (i.e., isolated, pattern, or widespread). The scope and severity classification relates only to skilled nursing facilities. The grid below provides a visual display of the scope and severity classification.
There are four severity levels.
Level 1 (A, B, C) is a deficiency that has the potential for causing no more than a minor negative effect on the resident(s). No actual harm with potential for minimal harm.
Level 2 (D, E, F) is noncompliance that results in no more than minimal physical, mental and/or psychosocial discomfort to the resident and/or has the potential (not yet realized) to compromise the resident’s ability to maintain and/or reach his/her highest practicable physical, mental and/or psychosocial well-being as defined by an accurate and comprehensive resident assessment, plan of care, and provision of services. No actual harm with potential for more than minimal harm that is not immediate jeopardy.
Level 3 (G, H, I) is noncompliance that results in a negative outcome that has compromised the resident’s ability to maintain and/or reach his/her highest practicable physical, mental and psychosocial well-being as defined by an accurate and comprehensive resident assessment, plan of care, and provision of services. This does not include a deficient practice that could or has caused limited consequence to the resident. Actual harm that is not immediate jeopardy.
Level 4 (J, K, L) is immediate jeopardy, a situation in which immediate corrective action is necessary because the facility’s noncompliance with one or more requirements of participation has caused, or is likely to cause, serious injury, harm, impairment, or death to a resident receiving care in a facility.
There are three scope levels: isolated; pattern; and widespread.
Scope is isolated (A, D, G, J) when one or a very limited number of residents are affected and/or one or a very limited number of staff are involved, and/or the situation has occurred only occasionally or in a very limited number of locations.
Scope is a pattern (B, E, H, K) when more than a very limited number of residents are affected, and/or more than a very limited number of staff are involved, and/or the situation has occurred in several locations, and/or the same resident(s) have been affected by repeated occurrences of the same deficient practice. The effect of the deficient practice is not found to be pervasive throughout the facility.
Scope is widespread (C, F, I, L) when the problems causing the deficiencies are pervasive in the facility and/or represent systemic failure that affected or has the potential to affect a large portion or all of the facility’s residents. Widespread scope refers to the entire facility population, not a subset of residents or one unit of a facility. In addition, widespread scope may be identified if a systemic failure in the facility (e.g., failure to maintain food at safe temperatures) would be likely to affect a large number of residents and is, therefore, pervasive in the facility.
The term "2567" is commonly used when referring to the document that contains the Summary Statement of Deficiencies and Plan of Correction. This form is used by CDPH to notify the health facility/provider of their non-compliance to federal or state regulations. In addition, this form is used by the health facility/provider to respond to CDPH with its corrective action plan and anticipated completion date.
A validation survey is a certification survey conducted in hospitals to determine if the “Conditions Of Participation (COP)” for participation for federal reimbursement programs (Medicare and/Medi-Cal) are being met by the hospital. The hospital must be in compliance with all applicable federal laws and regulations related to the health and safety of patients. These validation surveys are usually conducted at the approval of the federal Centers for Medicare and Medicaid Services (CMS) after an adverse event is reported and investigated and it has been determined that the event is a violation/deficiency of COP.
A deemed facility or provider is a facility that has been determined to meet Medicare “Conditions Of Participation” (federal regulations and laws) by virtue of their accreditation by an accreditation agency. These accreditation agencies are typically provider organizations such as the Joint Commission on Accreditation of Healthcare Organizations (Joint Commission or JCAHO), and American Osteopathic Hospitals (AOH) that have been deemed by CMS to determine their hospital members meet CMS “Conditions Of Participation” through their accreditation process.
Health care facilities and providers that want to participate in and receive payment from the Medicare or Medi-Cal programs must be certified as complying with the Conditions of Participation (CoPs), or standards, set forth in federal regulations. This certification is based on a survey conducted by CDPH L&C on behalf of CMS.
As an alternative, if a national accreditation organization has and enforces standards that meet the federal CoPs, CMS may grant the accreditation organization "deeming" authority and "deem" each accredited health care facility or provider as meeting the Medicare and Medi-Cal certification requirements. The health care facility or provider would have "deemed status" and would not be subject to the Medicare survey and certification process because it has already been surveyed by the accreditation organization.
Accreditation is voluntary and seeking deemed status through accreditation is an option, not a requirement.