
Antibiotics
An antibiotic is a medication that is used to treat bacterial infections. It works by either killing the bacteria or preventing its growth. Antibiotics can be life-saving. Antibiotics are not effective against viruses, such as those that cause the common cold or influenza.
What are bacteria & viruses?
 |
|
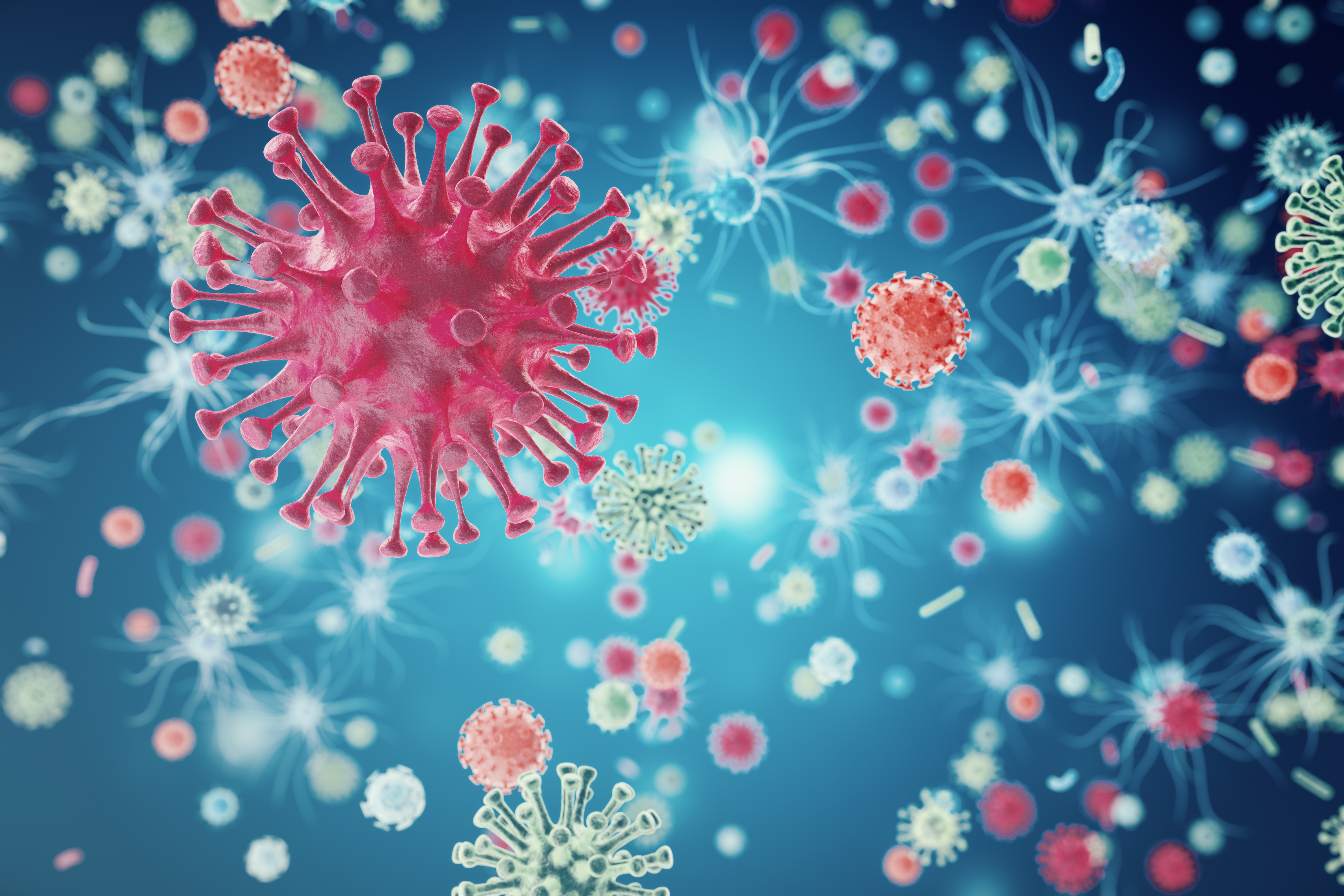 |
| Bacteria are microscopic, single-celled organisms that live in the intestinal and upper respiratory tracts of our bodies and in soil and water. Bacteria can live with and help humans and animals or they can cause infections. Bacteria can cause many different types of infections such as urinary tract infections, strep throat, and skin abscesses. |
|
Viruses are microorganisms that are smaller than bacteria and cannot grow or reproduce outside of a living cell. Viruses can infect all types of life forms. Viruses cause illnesses such as the common cold and influenza. |
What is antibiotic resistance (AR)?
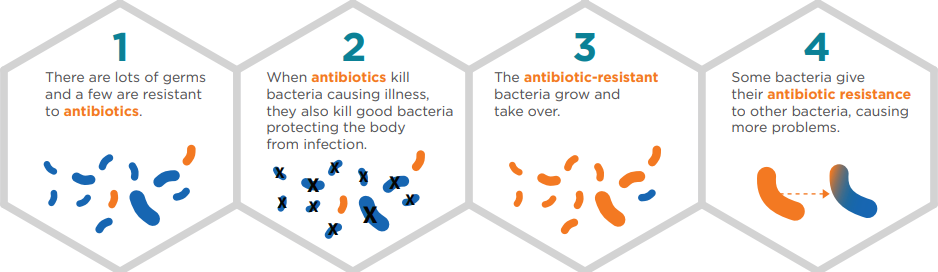
AR is the result of changes in bacteria that reduce or eliminate the ability of the antibiotic to kill bacteria that previously were able to successfully kill those bacteria and treat the infection caused. Exposure of bacteria to antibiotics encourages resistance to occur.
What is the connection between AR and the food that we eat?
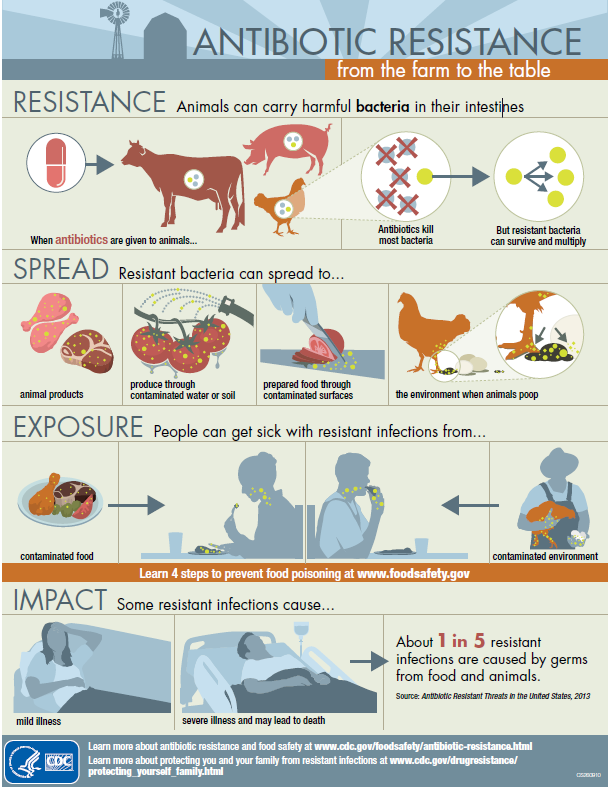
Antibiotics had been used to increase growth of farm animals. Giving antibiotics to animals will kill most bacteria, but resistant bacteria can survive and multiply. When food animals are slaughtered and processed, these bacteria can contaminate the meat or other animal products. People are exposed to the resistant bacteria when they handle or eat meat or produce contaminated with resistant bacteria or come into contact with animal poop. In the U.S., there are now laws to use antibiotics for animals only to treat infections.
Why should I care about AR?
AR is one of the most serious public health problems in the United States and worldwide and threatens to return us to the time when infections were not treatable and were often fatal. 30% of antibiotics are prescribed unnecessarily in doctors’ offices and emergency departments in the United States.
What can I do to help prevent AR?

Everyone can contribute to this effort. It is important for patients and healthcare providers to understand how to use antibiotics to minimize the risk of resistance.
-
Antibiotics save lives. When someone needs antibiotics, the benefits outweigh the risks of side effects or antibiotic resistance.
-
Antibiotics aren’t always the answer. Everyone can help improve antibiotic prescribing or use.
-
Antibiotics do not work on viruses, such as colds and flu, or runny noses, even if the mucus is thick, yellow or green.
-
Some infections such as ear infections, bronchitis, sinusitis will resolve without antibiotic treatment. Your provider will determine when antibiotics are indicated.
-
An antibiotic will not make you feel better if you have a virus. Respiratory viruses usually go away in a week or two without treatment. Ask your healthcare professional about the best way to feel better while your body fights off the virus.
-
Taking antibiotics creates resistant bacteria. Antibiotic resistance occurs when bacteria develop the ability to defeat the drugs designed to kill them.
-
If you need antibiotics, take them exactly as prescribed. Talk with your doctor if you have any questions about your antibiotics, or if you develop any side effects, especially diarrhea, since that could be a C. difficile (c. diff) infection which needs to be treated right away.
|
- Clean your hands regularly, especially before and after preparing food and touching animals.
- Get vaccinated
- Follow
CDC advice for food and water safety when traveling
- Purchase antibiotic-free meat and poultry
|
When should I be treated with an antibiotic?
Antibiotics hasten recovery and save lives when people have certain bacterial infections. When you have a bacterial infection, you should receive an antibiotic that is tested to treat that infection.
What precautions should I take when I am taking antibiotics?
If you need antibiotics, take them exactly as prescribed; do not skip doses. Talk with your doctor if you have any questions about your antibiotics, or if you develop any side effects, such as nausea, vomiting, headache, dizziness and especially diarrhea, since that could be a
Clostridioides difficile (C. diff) infection which needs to be treated right away.
When shouldn’t I take antibiotics?
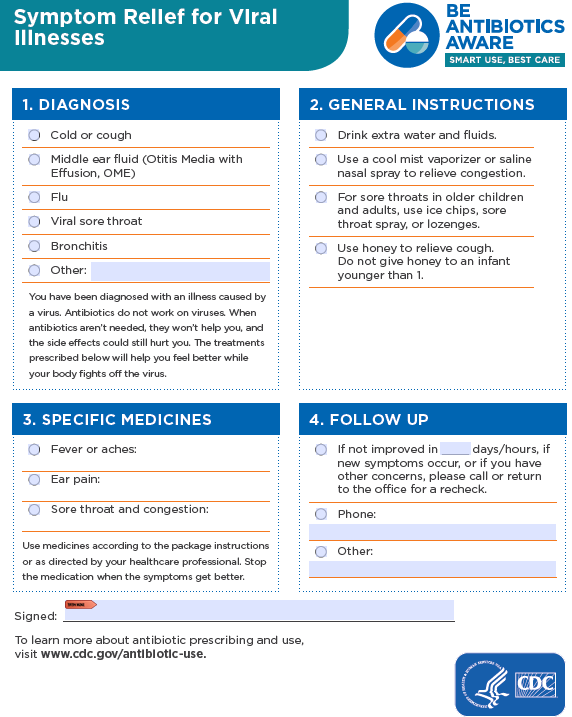

Antibiotics do not work on viruses, such as colds and flu, or runny noses, even if the mucus is thick, yellow or green. An antibiotic will not make you feel better if you have a virus.
Say No. Do not pressure your prescriber to treat you with an antibiotic. Ask for medications that will give you symptomatic relief. While antibiotics cannot treat infections caused by viruses, there are still a number of things you can do to relieve some symptoms and feel better while a viral illness runs its course. Over-the-counter medicines may also help relieve some symptoms.
- Get plenty of rest
- Drink plenty of fluids
- Use a clean humidifier or cool mist vaporizer
- Avoid smoking, secondhand smoke, and other pollutants (airborne chemicals or irritants)
- Take acetaminophen, ibuprofen or naproxen to relieve pain or
- Use saline nasal spray or drops
What is the CDPH HAI Program doing to help protect Californians from AR?
Studies have shown that use of antibiotics only when needed in all healthcare settings can reduce antibiotic resistance. CDPH has been engaged in several collaborative efforts throughout the state to reduce unneeded antibiotic use (Antibiotic Stewardship) by providing education to providers and patients and by tracking and containing highly resistant bacteria. The State of California requires all hospitals and skilled nursing facilities to have antimicrobial stewardship programs.
Additional AR Resources
HAI Program
For more information contact the HAI program at
HAIProgram@cdph.ca.gov